Vision Benefits

Regence BlueShield of Idaho contracts with Vision Service Plan (VSP) to provide the vision benefit. Coverage is included with enrollment in the medical plan. Refer to the vision plan documents below.
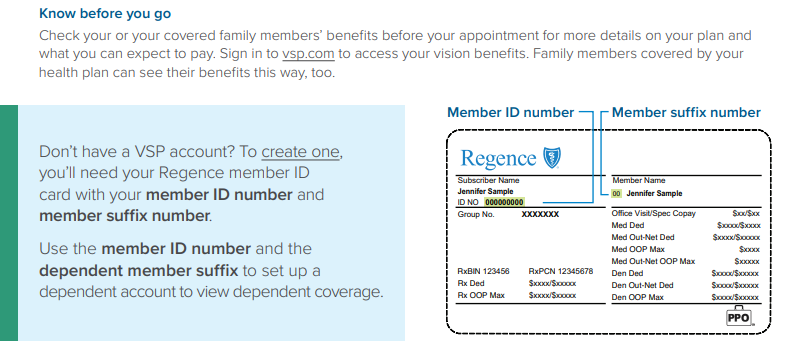
The links below provide information further detailing the State’s current vision plan.
FY27 Adult & Pediatric Vision Benefit Summary
FY27 [Coming Soon] Vision Booklet
FY26 Adult & Pediatric Vision Benefit Summary
FY26 Vision Booklet
Finding a VSP Provider – VSP
Resources line for contacting VSP at 1-844-299-3041
Vision FAQs
Do I have to use a VSP network vision care provider?
You can use the vision care provider of your choice. The advantage of using a VSP network provider is that VSP network doctors contact VSP to verify your eligibility, plan coverage, and to obtain authorization for services. Upon completion of the appointment, the VSP network doctor submits the claim to VSP for processing and VSP pays the doctor directly.
Will my VSP network vision care provider bill my insurance?
There are no claim forms to complete when you see a VSP doctor. VSP network doctors contact VSP to verify your eligibility, plan coverage, and to obtain authorization for services. Upon completion of the appointment, the VSP network doctor submits the claim to VSP for processing and VSP pays the doctor directly.
How do I submit a claim for a non-network vision care provider?
If you choose to see an out-of-network provider rather than a VSP Network Doctor, you will need to submit a claim to VSP for reimbursement.
Visit the Benefits & Claims section of the VSP website to submit a claim. You'll have the opportunity to upload receipts or submit them by mail. Please submit your itemized receipt(s) along with the out-of-network reimbursement form. VSP will reimburse you the allotted amount based on your benefits.
Do I have to use a VSP network vision care provider?
You can use the vision care provider of your choice. The advantage of using a VSP network provider is that VSP network doctors contact VSP to verify your eligibility, plan coverage, and to obtain authorization for services. Upon completion of the appointment, the VSP network doctor submits the claim to VSP for processing and VSP pays the doctor directly.
Will my VSP network vision care provider bill my insurance?
There are no claim forms to complete when you see a VSP doctor. VSP network doctors contact VSP to verify your eligibility, plan coverage, and to obtain authorization for services. Upon completion of the appointment, the VSP network doctor submits the claim to VSP for processing and VSP pays the doctor directly.
How do I submit a claim for a non-network vision care provider?
If you choose to see an out-of-network provider rather than a VSP Network Doctor, you will need to submit a claim to VSP for reimbursement.
Visit the Benefits & Claims section of the VSP website to submit a claim. You’ll have the opportunity to upload receipts or submit them by mail. Please submit your itemized receipt(s) along with the out-of-network reimbursement form. VSP will reimburse you the allotted amount based on your benefits.

